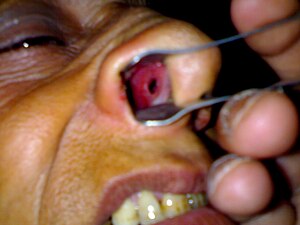
Nasal septum perforation
| Nasal septum perforation | |
|---|---|
 |
|
| Classification and external resources | |
| Specialty | pulmonology |
| ICD-10 | J34.8 |
| ICD-9-CM | 478.1 |
A nasal septum perforation is a medical condition in which the nasal septum, the cartilaginous membrane dividing the nostrils, develops a hole or fissure.
This may be brought on directly, as in the case of nasal piercings, or indirectly, as by long-term topical drug application, including intranasal ethylphenidate, methamphetamine, cocaine, crushed prescription pills, or decongestant nasal sprays, chronic epistaxis, excessive nose picking and as a complication of nasal surgery like septoplasty or rhinoplasty. Much less common causes for perforated nasal septums include rare granulomatous inflammatory conditions like granulomatosis with polyangiitis. It has been reported as a side effect of anti-angiogenesis drugs like bevacizumab.
A perforated septum can vary in size and location, and is usually found deep inside the nose. It may be asymptomatic, or cause a variety of signs and symptoms. Small perforations can cause a whistling noise when breathing. Larger perforations usually have more severe symptoms. These can be a combination of crusting, blood discharge, difficulty breathing, nasal pressure and discomfort. The closer the perforation is to the nostrils, the more likely it is to cause symptoms.
Septal perforations are managed with a multitude of options. The treatment often depends on the severity of symptoms and the size of the perforations. Generally speaking anterior septal perforations are more bothersome and symptomatic. Posterior septal perforations, which mainly occur iatrogenically, are often managed with simple observation and are at times intended portions of skull base surgery. Septal perforations that are not bothersome can be managed with simple observation. While no septal perforation will spontaneously close, for the majority of septal perforations that are unlikely to get larger observation is an appropriate form of management. For perforations that bleed or are painful, initial management should include humidification and application of salves to the perforation edges to promote healing. Mucosalization of the perforation edges will help prevent pain and recurrent epistaxis and majority of septal perforations can be managed without surgery.
...
Wikipedia
